As a nurse practitioner managing a Private Practice, implement these 5 strategies to help increase your bottom line.
After all, to continue providing services to patients, it’s a necessity, you must get paid for your time. With operating costs continuing their upward ascent, it’s vital to maximize reimbursement when you can. Yet, opportunities for Nurse Practitioners to maximize their private practice income are frequently missed. Omissions may result in lower reimbursements. Things like sloppy documentation and incorrect CPT codes can cause insurers to deny claims, or pay less than they otherwise would. Did you know that approximately 80 percent of medical claims contain errors?
To make matters more challenging, the large corporate Walk-in Clinics seem to be popping up on every street corner, and in every strip mall. This phenomenon is causing a more competitive environment for the small, Nurse Practitioner who wants to run their own business and provide value to their local community. It seems a perfect storm is brewing to make competing with the Corporate Healthcare Leviathan all the more difficult. So, In order to compete, providers need to be more nimble, think ‘outside the box, and place emphasis on ‘Service’ and followup. Providers also need to figure out how to get patients to choose the small clinic over the large corporate providers.
Large Corporate Providers might be able to scale their purchasing power, but they cannot scale the ‘patient satisfaction level’, like the way smaller clinics can. So, here are 5 ways a Solo Nurse Practitioner can maximize their private practice income to compete with the Corporate Laviathons, and best of all, Win!
#1 Empathetic Bedside Manner.
This is common sense, It’s called treating someone like you want to be treated. It’s empathy, its compassion, its winning people over with kindness. I remember my last experience with the ‘Corporate Urgent Care” where I left feeling under-appreciated, rushed, and all I was doing was contributing my good “Blue Cross Blue Shield Policy”, to their bottom line. The 99213 I received would pay them in 14 days, with no ‘self-pay balance’ for which they needed to send a statement on. The 15 minutes they spent with me, likely netted them $150. So, In the world of medical Insurance claims filing, I was the “Holy Grail”. I get that my 15-minute office visit, was used to offset the cost of the uninsured patient sitting in the waiting room, but at least treat me like your glad to see me. I’m not asking for preferential treatment of course, just be a little less obvious you’re trying to rush me out.
In the end, showing empathy and compassion, will go a lot farther for the Nurse Practitioner who is running their private practice, and will ultimately pad your bottom line.
#2 Communicating…Outside the Exam Room.
 No one says you can’t mail your Blue Cross patients, a reminder that you do Well Checks, Sports Physicals, and Xrays. No one says you can’t email your Soon-to-be Medicare Patients a Medicare and You Pamplet. And sending your Blue Cross Patients a birthday card, well that goes back to the aforementioned #1 ‘Empethetic Bedside Manner’ and the “Winning people over with kindness” montra. Communication is still a virtue many people appreciate. So, the age-old challenge becomes, how do providers stay in communication with patients once they leave their office?
No one says you can’t mail your Blue Cross patients, a reminder that you do Well Checks, Sports Physicals, and Xrays. No one says you can’t email your Soon-to-be Medicare Patients a Medicare and You Pamplet. And sending your Blue Cross Patients a birthday card, well that goes back to the aforementioned #1 ‘Empethetic Bedside Manner’ and the “Winning people over with kindness” montra. Communication is still a virtue many people appreciate. So, the age-old challenge becomes, how do providers stay in communication with patients once they leave their office?
Here are a few methods of communication you should consider:
Email marketing:
In the age of digital, correspondence with patients can be cheap, but often time less effective. We’ve all become calloused by email bombardments and mail solicitations to get us to change our behavior. So, reaching your desired outcome with email and ‘snail mail’, is like throwing spaghetti against the wall and seeing what sticks. But, it’s worth it, because some of the spaghetti is bound to stick! So do not overlook this with obtaining patient email addresses, especially younger ones. Not for the purpose of providing any health information, we all know that, but to communicate with your patients. Keep in mind, you’re solicitation is “warm”, they are likely to click on your email, because they know and trust you.
So how does a Nurse Practitioner gather email addresses?
First of all, have your front desk say to patients at registration: “Please include all means of contact, including email, in case the doctor needs to contact you”.
This is crucial, and most patients are willing to provide their email address when asked this way.
The hidden value of email lists.
If you ever go to sell your business, think of it, what’s more valuable a practice with 2000 active patients, or a practice with 2000 active patients and 20,000 email addresses. You guessed it, the latter. According to the Privy Network, each email address collected can be worth up to $15.23 in sales. This obviously differs from Industry to Industry, and Healthcare may be an anomaly, but even if one email could generate $10 in income, on 2000 patients, that’s an extra $20,000 per year.
Add a Blog to your practices Website, and create content:
Again, this is a huge value add to the overall worth of your practice. A blog and a website are Intellectual property, and people pay big money for this kind of intellectual property. Smartblogger posted this blog article about 10 bloggers making over a $1,000,000 per year from their Websites. A blog raises your profile in search engines. Websites with keywords that appear on the first page of Google aren’t there by mistake, they’ve created content related to the specific keyword searched. A blog with 1000 ‘Search Engine Optimized” keywords, may be able to add another $100,000 per year of value, to your practice. Content creation can be hired out, through websites like Fiverr.com and Freelancer.com. So this means you don’t have to have a “New York Times Writer” on staff, just someone with a willingness to write content and who knows a little about Search engine optimization.
# 3 RV-U Must monitor production!
RVU’s, commonly known as Relative Value Units, or as we like to call it ‘Restoring Vested Urgency’. In a Nurse Practitioners Private Practice, it’s a great way to incentivize the providers in your clinic.
It takes altering the mindset of providers at a medical facility from ‘wage-earner’ to ‘producer’ and this almost always takes enticement. Enticement can be many things, but in the case of RVU’s, it’s of a monetary nature. Restoring Vested Urgency is simply getting providers to be ‘vested’ in the “mission” and rather than thinking like a wage-earner, for them to think like business owners. The “mission” is to care for people, first and foremost, but it’s also to make a living. In order to make a living, and keep up with inflation, you need to make a profit year after year.
So, how do we make a profit? Simple economics of course, take in more than you pay out. But, but, its simply not that simple! As you know there are a lot of moving parts to running a medical clinic, some of which are out of your control. One of the parts you can control, is how you pay the providers in your clinic, and the best way create a “Vested Urgency” is to implement an RVU bonus program.
What are RVU’s and how can they be used to Incentivize?
People are inevitably going to do what is convenient…..to them. Sometimes It’s more conveinient to give the patient a shot when you want to hurry off to your lunch date, rather than an office visit and subsequent 99213. But what if that 99213, was tied to a RVU bonus? I promise it will change providers behavior, it will make them more competitive, and they may end up deciding, well low and behold, lunch can just wait a few extra minutes.
If you’re planning to implement an RVU Bonus Program, please don’t forget to do these:
- Track the RVU’s. Seems simple, but without a tracking mechanism it’s useless knowledge. Choose a Practice Management program or billing company which can offer RVU Tracking like we do at Medlink Services.
- Make bonus payments monthly not quarterly: This way the provider remains ‘engaged’, and by receiving feedback on a regular monthly basis, it will reinforce Productive Behavior.
Quarterly is too long. Think of “the carrot and stick” analogy; you wouldn’t have a stick that was so long, the horse mistook it for beets, or mushrooms, or some other undesirable vegetable, would you?
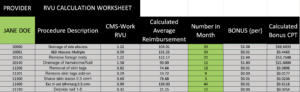
Here is the RVU Tracker we use with some of our clients, if you’re interested in a full copy for your practice, please contact us.
#4 Know Which E/M code to use… and don’t be afraid to use it
The Evaluation and Management (E/M) service is the most common service provided by nurse practitioners. Most patient visits require the use of an E/M code. Therefore, it is essential to choose the right code. However, incorrect evaluation and management codes are often selected, either out of fear of your; not substantiating the chosen level of care, or maybe the fear of being audited. Either way, you’ve miscoded, which is often the result of loss revenue, sometimes significant losses in revenue. In 2012, the American Academy of Professional Coders (AAPC) conducted a review of more than 60,000 medical billing audits. More than a third of the records examined were under-coded. This represents an average loss of $64,000 in revenue per provider. You can avoid this by selecting the correct E/M code.
How To Choose The Right E/M Code
Complexity is the key to choosing the correct E/M level. These codes are based on the presenting problem, patient history, examination, and medical decision making. Here is a handy chart to help you select the correct code.
#5 Implement a robust Patient Payment process!
First and foremost, teach your front desk how they can accurately verify when a returning patient, has a balance. The front desk must be confident in this, or they simply won’t ask. So, does your system clearly show, when a balance is due?
Nurse Practitioners typically generate 20-25% in Revenue from Patient Payments. So, A drop in Patient Payments to 10%, can potentially put a Nurse Practitioner out of business. You must have a Robust Patient Payment Process, like Medlink Services has.
Here are some tips to help your staff build confidence on asking for payment at the time of service.
Not asking a returning patient to pay an old balance is essentially giving them the authority to; not pay for this visit.
Automate your Statement Process
Have a consistent and immediate method for moving accounts to patient balance when both the primary and secondary payers have paid. The longer time lapses, the greater the opportunity the patient has to; Move or Change their Phone Number.
Time is not on your side:
It is said that collectability drops by 80% once the patient leaves your office. And, not having the correct address or phone number, increases this immensely. The longer time goes by from when the patient leaves your office to the when they receive their first statement, only hurts your chance of payment.
When asking for payment, teach your staff to ask “how” they want to pay today, not “will” they pay today. Use statements like “We take Visa, Mastercard, or Discover, which would you prefer? “. Or, “your total is $30 today, do you want to write a check for that?”.
Making a firm statement, then asking for payment will put your staff member in a position of authority, and patients are more likely to pay when the message is delivered by someone in a position of authority. This practice will certainly increase your patient payment revenue.
Remember; your Practice is a Business, businesses succeed when they are profitable. These 5 strategies will certainly help your Nurse Practitioner Private Practice Income.
Photo Credit: Medical Economics