A Family Practice Physician must decide between starting a solo practice or becoming a hospital employee. Here is why starting your own practice may temper Physician Burnout.
You’ve made it through the rigors of Medical School, Residency, and perhaps even a fellowship, and now is the time to decide which family practice physician opportunity is the best for you and your family. In this post we will be discussing the merits of starting a solo family practice and bucking all negative Physician Burnout Statistics.
It’s hard to compare being a private practice physician and a hospital owned physician, because in my eyes it wouldn’t even be a comparison. It really comes down to how you value autonomy and freedom, which I value as being of the utmost importance. Yes, even over money.
We’ve helped many Family Practice Physicians be successful using our medical billing service, so we know it can be financially successful. But, there are challenges with Employees, Taxes, Expenses and liability, which can be passed on to the hospital if you are an employee. So I get it. As a physician exploring ‘one road or the other’ you have to weigh your options, and determine what is best for you, at this very time.
The Top 5 benefits of a being a Private Family Practice Physician
#1 Enjoying the Freedom and Autonomy to be your own boss.
As I stated this is high on my priority list, while it may not be for others. But, having the financial autonomy to work when you want to, and with who you want to, is truly hard to even compare. Being your own boss as a Private Practice Physician comes with financial risk, which you may not have as an employee of a hospital. That said, being a hospital owned employee, comes with Opportunity Risk, mainly by the fact that you will never know what you could become, if you choose the ‘safe’ route of being a hospital employee.
#2 Choosing which types of patients you want to treat.
Do you want to help the elderly, or perhaps the indigent, or a mix of all. As a Private Practice Physician, you get to decide; you’re the boss. Medicare is a great payer, and typically pays in 14-16 days. Blue Cross is also a great payer, and many people with Blue Cross are employees, with jobs, higher credit scores, and the means to pay their self-pay balance. You may not want to see Medicaid Patients, which is not as good of a payer as Blue Cross or Medicare. So, as a Private Practice Physician, you have that complete autonomy to decide who and when to see certain patients.
#3 Family Practice Physicians have the ability to make as much, or little as they want.
Hospital owned physicians are like military GI’s, or otherwise referred to as ‘Government Issue’. This is a term which means when you join the military, you are indeed property of the government. Hospital owned physicians are essentially owned by the hospital. They tell you when you’re on call, when you take vacation, and even how close to the hospital you need to live. Sounds like they own you, huh? Seems like you trade your autonomy for a hospital paycheck when you are a hospital owned physician.
#4 Complete autonomy to make the necessary business decisions.
Do you want to implement a 401k for your employees, if so which fund manager do you use. Do you want to change healthcare coverage because your group deductible keeps going up? These are the business decisions, you as a Solo Practitioner has the complete autonomy to make.
#5 The thrill of growth and the agony of defeat.
The thrill of growth is understandable, but the agony of defeat? How is this a benefit? Well, running a business comes with peaks and valleys, and the agony of defeat helps you maintain humility. Often times you learn more from defeat. As a result, you grow and learn, and respect the process more. This phenomenon shouldn’t be overlooked.
Lastly, Physician Burnout is real! The pandemic only exacerbated this and in order to sustain a long career in healthcare today, it’s important to resist physician burnout. One way of doing this while still serving patient needs is by building a business, one which can offer a different area of fulfillment, and one which allows you more autonomy.
Here are some recent Physician Burnout Statistics and the most vulnerable medical specialties at risk.

Statistics provided by Medscape; Death by 1000 cuts; Medscape National physician burnout and suicide report 2021.
Here are the top 5 things to consider if you plan to start a medical practice.
#1 Choose a location which allows you to keep your expenses low and your exposure high.
According to the Bureau of Labor and Statistics, 17.4% of businesses fail in the first two years, but thats an 83% survival rate. We can work with that! And, according to Investopedia’s post; The top 6 reasons new businesses fail lists #4 as bad location, internet presence and marketing. Bad location can be a few things; such as not enough exposure, cost of rent is too high, and even something as seemingly mundane as; parking. If you have to park too far from the office, your disabled or elderly patients may not come. This ,as you may have guessed, can be the curse of death to any new business.
#2 Pay your Medical Staff well.
The survival of any business comes down to revenue verses expenses, and while this may sound simplistic, it’s often more difficult to manage for the long term. Paying your Medical Staff well is important, but paying them too well can improve your chance of failure. You will experience high turnover with receptionists, so finding a family member to work that position in the beginning, is ideal. Pay the members of your medical staff who are considered; revenue generators, well. This includes; Nurses, billers, and coders. Or, outsource this to a boutique billing company such as Medlink Services, who is willing to be paid on a percentage of revenue which is brought into the practice.
#3 EMR vs EHR Software.
The Electronic Health Record Market is confusing, it’s fraught with so many options who offer software programs with slick bells and whistles, which in many cases are un-necessary to the viability of your practice. Knowing the difference between an (Electronic Medical Record) EMR vs an EHR (Electronic Health Record) can be; ‘make or break” important!
Here are 5 important differences between an EHR and an EMR.
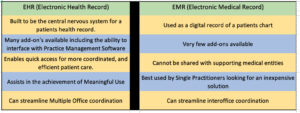
Investing in an expensive EHR Software Program when first starting out as a Family Practice Physician may be a disadvantage. Many EHR software providers also offer billing as an add-on service. Often times these are 2 independent software companies; the EHR Software and the Practice Management Software, which are then married together with an interface. The challenge with these is again, Autonomy, or lack of Autonomy.
If for instance, you like your EHR, but don’t think the company is doing a good job with your claims follow-up, then its more complicated to change the staff who is doing your billing because they are all tied together.
Or, if for instance you have software issues, which take a while to get resolved, and meanwhile your claims are stuck or unable to be billed out, and your money suffers. This is why Medlink Services is a ‘Software Agnostic’ billing company who welcomes any EHR, or EMR you desire.
#4 Success will depend on vigorous public outreach.
Running any successful business depends on the public’s perception of the business. This is no different for a Family Practice Physician’s business. Public outreach creates a connection with the community, which is exceptionally important. Sponsoring events, sitting on boards, working at the local food bank, are all examples of public outreach that can enable you to gain positive exposure and will eventually lead to more business. It’s great to do for your business, not to mention, its great to be able to serve the public in a selfless manner.
#5 Never forget you are building a tangible asset.
It’s true, the more ‘sweat equity’ you put into building your Private Physician Practice the more it becomes worth to someone in the future. You may decide to sell your practice one day and its value will matter. A Tangible Asset is something of value that you can see, touch, and feel. And, A private medical practice falls into that category. There will always be a value to a medical practice, and like most other tangible assets, this value increases over time.
So, if you are a Family Practice Physician evaluating between opening your own clinic or becoming an employee of a hospital, we hope this post helps you understand the value of owning and building a long-term tangible asset. Owning a business is rewarding, and is truly a lifestyle, rather than a job.



